When the World Health Organization declared the Ebola epidemic over on November 7, 2015, about 40% of the 8,704 people infected had died. The country’s health system, or what was left of it after a decade of civil war that ended in 2002, was ailing, too. Some health workers had become ill or left, leaving untrained volunteers in their stead. Piles of unused donated products were strewn in cramped storage spaces or sat on floors in health facilities, passing their expiration dates unnoticed. The latter would later be burned under uncontrolled conditions, spewing smoke and fumes in the open air. There were also communication challenges from the central government to health facilities and weak inventory control, and stock-outs of essential medicines were common.

These are symptoms of a health system that was in crisis long before Ebola– it just took a deadly epidemic to unmask them, says Murtada Sesay, Country Project Director in Sierra Leone for the USAID-funded Systems for Improving Access to Pharmaceuticals and Services (SIAPS) Program. A native of the country, he’s worked on supply chain operations for decades for a number of UN agencies.
“[Ebola] brought to light the weakness in the pharmaceutical sector. If you look at the epidemic, there were a lot of problems—not knowing where the pharmaceutical products were, why they weren’t getting to people, and who needed them,” he says.
SIAPS started working in September 2015 on a special project, funded by USAID, to help rebuild Sierra Leone’s pharmaceutical system and ensure access to critical medicines and related products. Sesay teamed up with Gabriel Daniel, a SIAPS Technical Lead, and local staff on a plan for the overhaul.
Advising institutions, coaching managers
The blueprint for rebuilding the system involved far-reaching activities, ranging from establishing and clarifying central leadership roles at the Directorate of Drugs and Medical Supplies of the Ministry of Health and Sanitation, to promoting accountability of local facility managers. A three-day workshop in Freetown capacitated public sector pharmacy managers from around the country in the basic practices of good leadership, management, and governance to help them identify challenges, such as system and budget constraints—and to lead their teams in handling them.
Access to medicines alone doesn’t guarantee optimal health outcomes, however; a sound pharmaceutical system also makes sure available medicines are safe and appropriately used. SIAPS helped four hospitals set up drugs and therapeutics committees, which help manage medicine selection, evaluate prescribing, and promote evidence-based medicine use throughout their facilities. Five more hospital committees are soon to launch, with plans underway to work with all 24 public hospitals in Sierra Leone. The program is also working with a national task force on a larger plan to combat antimicrobial resistance, a growing global threat.
Working “at the last mile”
The second critical piece of the health system reboot was to get health commodities moving. SIAPS introduced a Continuous Results Monitoring and Support System (CRMS) framework, with each of the country’s 13 districts—and 1,000 of 1,300 health facilities—reporting on disease morbidity, medicine consumption and availability, use of inventory tools, and staffing. District health leaders meet regularly and plan activities based on data from the reporting. Distribution and storage in local health facilities got an overhaul, too.
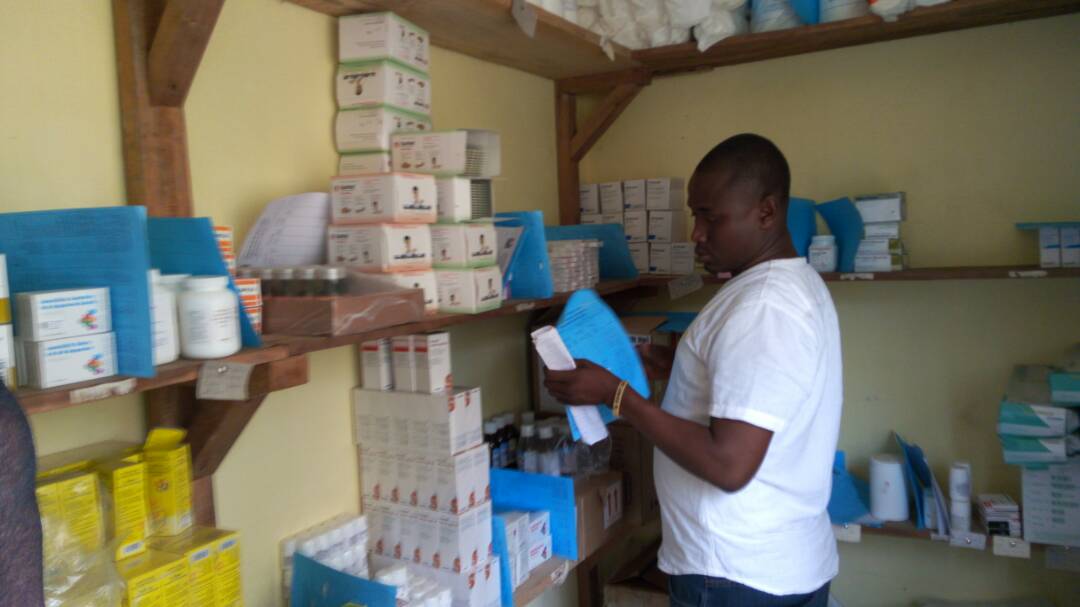
“Empowering local communities for sustainability is one approach that I admire . . . and that is the strategy that we have applied in the SIAPS Program countrywide,” says Marie Ibranatu Kolipha-Kamara, a pharmacist with the local SIAPS team. “We’ve been working with the foot soldiers in the field to build capacity, strengthening the system starting with the lowest level, while setting the platform for the upper level to be able to manage and make informed decisions for better health outcomes.”
New tools and technology, such as an electronic information system for public sector pharmacies, are helping health facilities and district teams make better decisions on procuring and allocating pharmaceutical products. SIAPS trained a national committee and seven technical working groups (TWGs) on how to use Quantimed, Pipeline, and QuanTB software for forecasting and supply planning of health commodities. The Free Health Care TWGs then planned procurement of supplies for the President’s Free Health Care Initiative to be funded by the Department for International Development (DFID) and USAID, targeted at pregnant women and children under five, for 2017 and 2018 on the basis of the results.
The process was a breakthrough for evidence-based planning, the staff says. “At the central level, the opportunity of being able to know the stock status situation in the country and also quantifying the volume of expired commodities to create storage space for usable products has helped in decision-making processes,” says Kolipha-Kamara.
SIAPS also developed a graphic display dashboard for an electronic system that provides real-time access to commodity and patient information, helping district- and central-level workers easily monitor stock levels at health facilities and district and central medical stores.
A can-do attitude
The team also needed a dogged mindset. Solving urgent issues when human resources and infrastructure are lacking often requires “grabbing a low-hanging problem first,” as Gabriel Daniel puts it, which can have a big impact on best practices and pave the way for larger-scale activities, such as coming up with a treatment register that’s easier and quicker to fill out to fully capture morbidity and medicine consumption data, or building pallets from locally available tree twigs to properly store medicines off the floor, which otherwise exposes them to pests and dirt from the floor.

Though only 18 months in, the SIAPS staff says the system is already considerably stronger.
“The SIAPS Program is a household name now in the health sector in Sierra Leone, starting from the central directorates and program and other implementing partners, to the district health management team, to the hospitals and peripheral health units. The health workers feel that the SIAPS Program is geared towards strengthening their system by mentoring them and making use of available structures and human resources. These are what I call sustainability strategies,” Kolipha-Kamara says.
Find our technical brief on strengthening the pharmaceutical system in Sierra Leone after Ebola here.

