One of the world’s oldest diseases, malaria claimed 1.2 million lives at its peak in 2004. Today, with proven prevention and treatment strategies, nine countries have now eradicated malaria. However, malaria still claims more than 400,000 lives each year—mostly children under the age of five in sub-Saharan Africa.
The costs of malaria do not stop at the immense loss of life; the disease also places a great financial burden on individuals and health systems alike. Up to 40% of public health spending in malaria-endemic countries goes toward treating the disease, and case management alone has cost Sub-Saharan Africa US $300 million each year since 2000.
Efforts to scale up anti-malaria interventions around the globe have shown great success in fighting malaria in recent years. Between 2000 and 2015, malaria mortality rates fell by 60% globally, while incidence rates fell by 37% in the same period. This progress has shown that elimination of malaria is possible; however, as the world’s population grows, more people will be living in areas where developing malaria is a persistent threat that will place additional strains on health systems. Furthermore, obstacles like unrest, climate change, drug resistance, and other disease outbreaks like Ebola represent barriers to achieving long-term, sustained control and elimination of malaria.
THE SIAPS APPROACH
Accelerating progress and scale-up of proven malaria interventions requires addressing systems-level challenges that further exacerbate the existing threats to malaria control. Increasing availability of medicines, for example, requires a strong supply chain; however, ensuring equitable access, transparent and accountable management, rational use, and appropriate surveillance of those medicines, requires a strong pharmaceutical system as a whole.
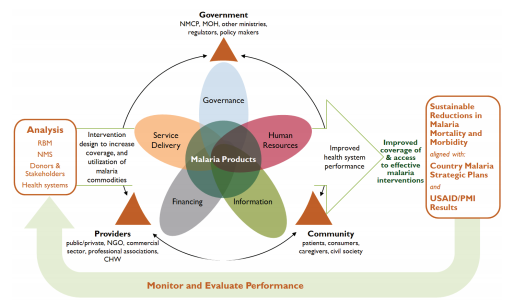
Since 2011, the USAID-funded Systems for Improved Access to Pharmaceuticals and Services (SIAPS) Program has taken a systems-strengthening approach to improving health outcomes. SIAPS Program’s anti-malaria interventions are rooted in the World Health Organization’s health system building blocks to strengthen the components of pharmaceutical systems which support expanded, equitable, and sustainable access to medicines and pharmaceutical services.
While working to control malaria in countries supported by the President’s Malaria Initiative (PMI), SIAPS staff have faced many similar challenges, even while working in very different environments and with different governments. From these common experiences, SIAPS Program has taken away key lessons that will continue to guide anti-malaria interventions.
LESSONS LEARNED
Coordination, at all levels, is a necessary but often overlooked contributor to strong systems. In every country where SIAPS is supporting PMI’s efforts to control malaria, and in all building blocks, efforts to coordinate across donors, implementing partners, government agencies, and disciplines, have been the foundation for more effective, efficient, and streamlined activities, processes, and systems. Coordination doesn’t just happen at the central level, but rather, across all levels of the pharmaceutical system.
While SIAPS has seen the benefits of pharmaceutical technical working groups and national quantification committees in optimizing procurements of antimalarials and ensuring a continuous supply of medicines, coordination that happens at the depot or hospital levels has also shown tremendous value in maintaining standards and processes not only down to the last mile of distribution, but also through prescribing, dispensing, and use.
Effective partnerships pave the way for scale-up of best practices. While working to shore up collaboration and coordination of our local counterparts, SIAPS has also endeavored to leverage effective partnership with other implementing partners to diffuse best practices and scale up effective interventions. In South Sudan for example, after a successful pilot of clearing out many storage facilities, a process known as dejunking, SIAPS developed guidelines which enabled the process to be replicated in other provinces and helped ensure that new products being procured could be distributed and stored in a proper manner.
Similarly, in the Democratic Republic of Congo (DRC) and Guinea, after several successful rounds of EUV, the Global Fund decided to adopt the survey in the provinces where it was supporting malaria control efforts and has asked SIAPS to support expanded EUV surveys in Global Fund-supported provinces and zones. In DRC, where malaria remains one of the top causes of death, this type of partnership is allowing the EUV survey to give ever-more accurate snapshots of the supply chain and availability of malaria commodities.
Making data easier to use drives effective decision making. While efforts to increase data availability and quality are vital and ongoing in all PMI-supported countries, some countries like Mali are going one step further and learning that when data are available, there are ways to ensure that the data are centralized, synthesized, and presented in ways which enable and promote more effective decisions and actions.
Through the PMI-supported web-based dashboard OSPSANTE, SIAPS has helped make supply chain data available to all relevant stakeholders, from the national level down to the province and facility level. Its interactive design and highly customizable reports allows in-country stakeholders to quickly access real-time information needed for decision making, and even flags potential issues before they arise to prevent stock-outs of life saving commodities. The ability to use data in this way has catalyzed accountability and demand for more data, as OSPSANTE helped to spur an increase of reporting rates and continues to add to the number of facilities contributing data.
Even small and incremental steps toward stronger systems can build resiliency. Strengthening pharmaceutical systems is a collaborative, stakeholder-driven, and incremental process – a process which is sustained by fostering country ownership and engagement. Although strengthening systems takes time, several PMI-supported SIAPS countries have seen how even small changes which fortify processes, policies, and people have resulted in demonstrably stronger systems.
In Guinea, for example, where SIAPS helped to overhaul the LMIS system for malaria commodities, reporting rates remained high, even as the country struggled to manage the Ebola outbreak. Regular reporting continued largely because the LMIS was rooted in mechanisms which promoted accountability, feedback, and ownership. These factors, combined with leadership from the NMCP, ensured that the LMIS continued to function, even in a time when the larger pharmaceutical system was in crisis.
Going forward, these lessons will resonate with SIAPS Program staff and their partners as they continue fighting malaria around the world. Implementing effective partnerships, closing information gaps, and improving coordination across health systems will continue to inform strategies for control and prevention, helping the champions of the global fight against malaria to end malaria for good.

